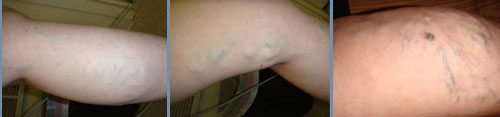
A significant number of Americans, particularly women, experience the discomfort associated with spider and varicose veins. These conditions manifest as swollen, protruding veins that often lead to leg pain. Individuals affected by these veins commonly find themselves hesitating to wear shorter clothing due to feelings of embarrassment concerning their appearance.
At Westchester Surgery P.C., we recognize the impact of spider and varicose veins on both physical well-being and emotional confidence. Our commitment to providing exemplary healthcare is underscored by our utilization of cutting-edge technologies in the diagnosis and treatment of these venous conditions.
Through a comprehensive approach, our skilled medical professionals tailor personalized solutions to address individual needs and restore patients to a state of optimal health. By choosing Westchester Surgery P.C., you are opting for a team dedicated to delivering top-tier medical care with a focus on innovative methodologies.
Allow us to guide you through a journey of diagnosis, treatment, and recovery, empowering you to reclaim the confidence that is rightfully yours. Trust us to assist you in regaining both physical comfort and confidence through advanced medical interventions tailored to your specific needs. We are here to help you navigate a path towards renewed well-being and self-assurance.
